In ophthalmic surgery, where micrometers define success, infection control is paramount. Even minor lapses can lead to devastating outcomes like endophthalmitis. Maintaining sterility is not only a protocol — it’s a culture of vigilance.
The Unique Challenges of Ophthalmic Surgery
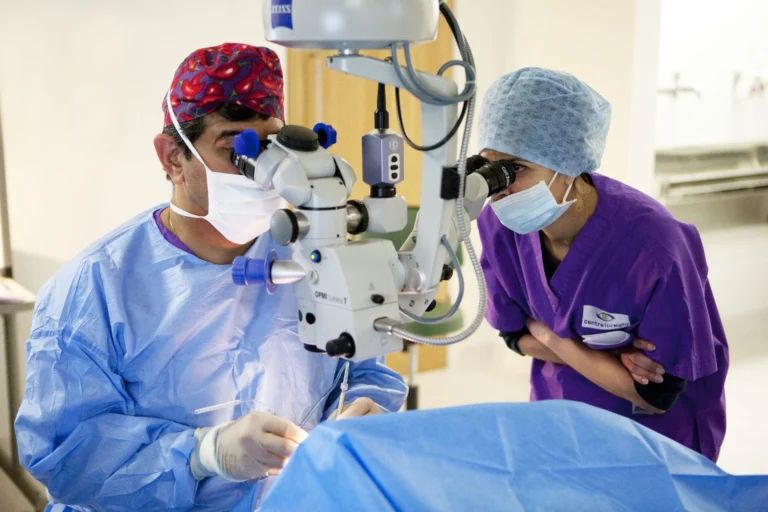
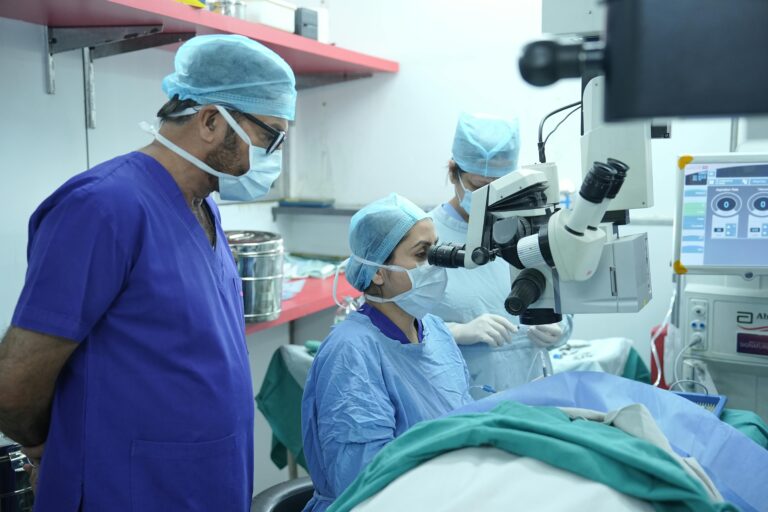
Ophthalmic procedures are typically short and involve small incisions, yet the stakes are high. The eye’s limited immune defenses make it particularly vulnerable to postoperative infection. Additionally, high surgical volumes demand efficient turnover without compromising sterility.
Preoperative Preparation
Meticulous preoperative antisepsis begins with povidone-iodine irrigation, the gold standard for ocular surface disinfection. Lashes are isolated, and sterile draping minimizes contamination risk. Surgeons should ensure proper hand hygiene and gowning protocols before every case.
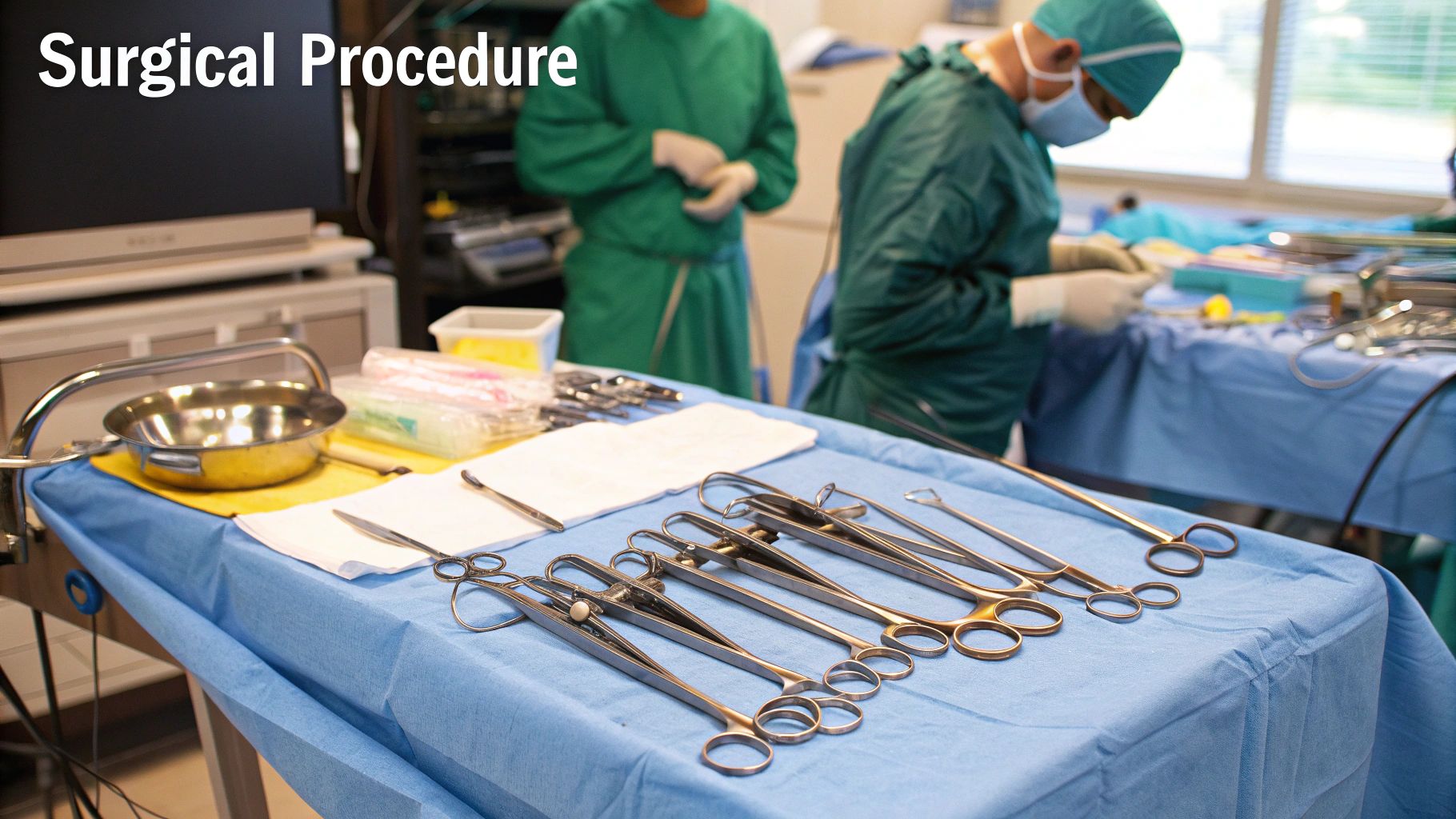
Instrument Sterilization and Handling
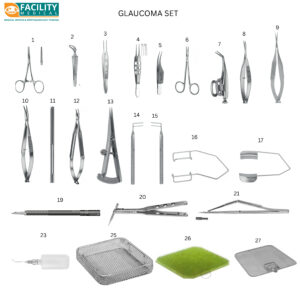
All reusable instruments must undergo complete cleaning, ultrasonic washing, and autoclaving. Single-use instruments and disposables (like cannulas and tubing) are now common to avoid cross-contamination. Surgical trays should be covered until immediately before use.
Environmental Control
The ophthalmic operating room must maintain:
- Positive air pressure
- HEPA filtration
- Controlled temperature and humidity
- Strict staff traffic flow
Periodic microbiological monitoring helps ensure environmental safety.
Antibiotic Prophylaxis
Intracameral antibiotics such as cefuroxime or moxifloxacin at the end of cataract surgery have significantly reduced infection rates. Topical antibiotics may supplement but should not replace proper asepsis.
Postoperative Education
Patient education is equally important — proper hygiene, medication adherence, and prompt reporting of symptoms can prevent complications.
Conclusion
Infection control in ophthalmic surgery is a continuous, team-wide responsibility. Adhering to meticulous aseptic protocols safeguards not just surgical success, but the vision patients trust us to protect.