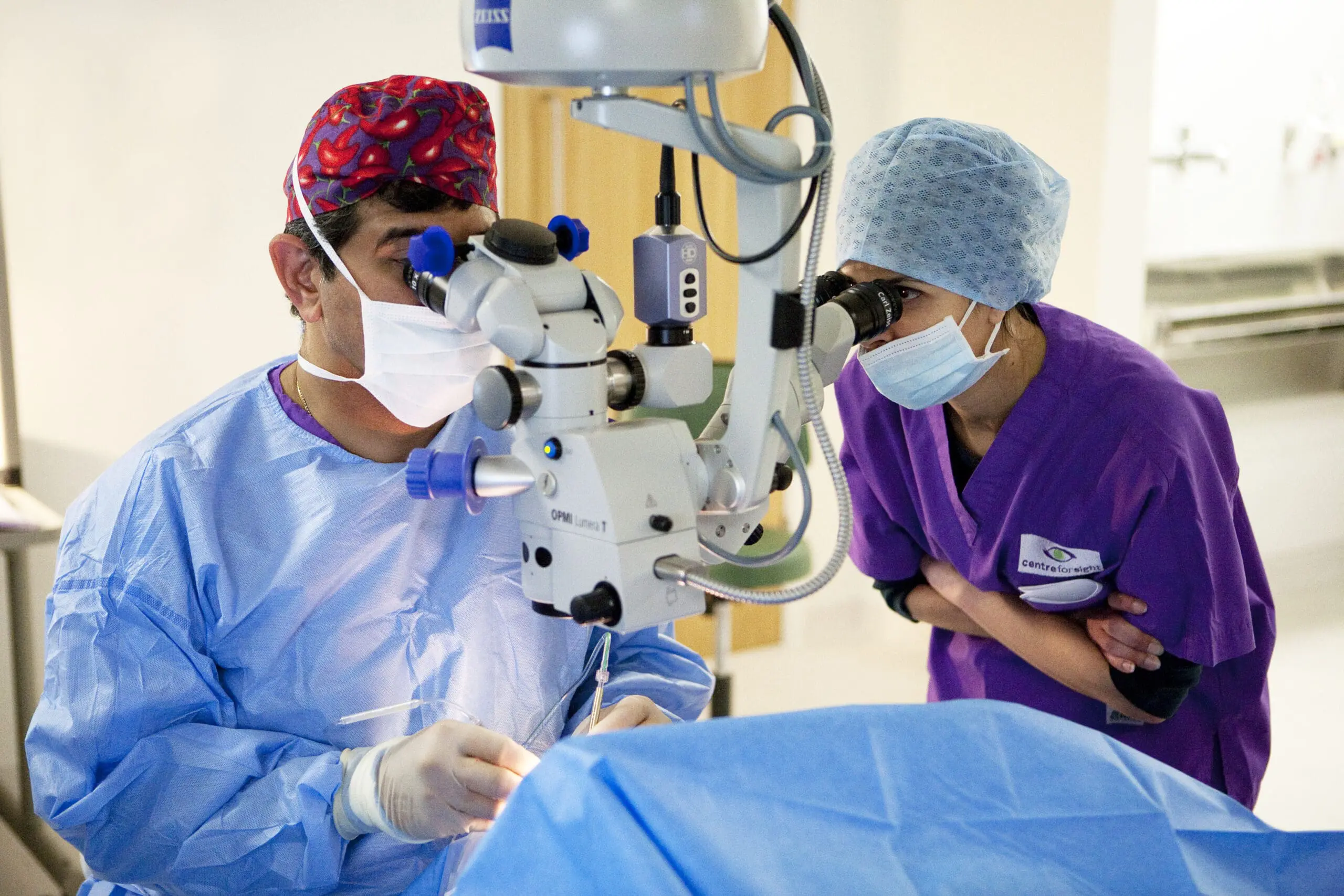
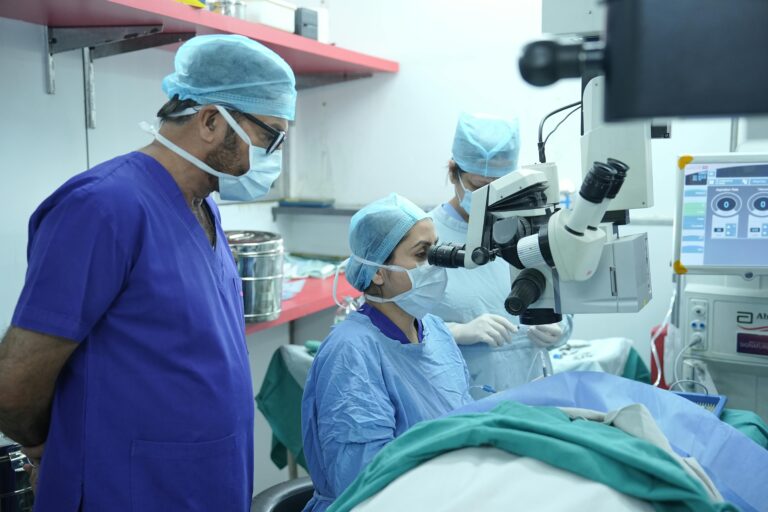
Glaucoma remains one of the leading causes of irreversible blindness worldwide. While medications and lasers are the first line of treatment, surgery plays a crucial role when intraocular pressure (IOP) cannot be controlled otherwise. The past decade has seen a revolution — the rise of Minimally Invasive Glaucoma Surgery (MIGS).
Traditional Glaucoma Surgery
Conventional options like trabeculectomy and glaucoma drainage devices (GDDs) remain highly effective but carry risks such as hypotony, bleb leaks, and infection. Although reliable, they often require intensive postoperative care.
The Emergence of MIGS
MIGS was developed to fill the gap between medications and traditional surgery — providing moderate IOP reduction with superior safety and faster recovery. These procedures use micro-incisions and target the natural aqueous outflow pathways.
Types of MIGS Procedures
- Trabecular Meshwork Bypass: Using stents like iStent or Hydrus to enhance outflow through Schlemm’s canal.
- Suprachoroidal Shunts: Divert aqueous humor into the suprachoroidal space.
- Subconjunctival Approaches: Devices such as the Xen Gel Stent create a controlled filtration pathway.
Advantages of MIGS
Compared to traditional surgery, MIGS offers:
- Minimal tissue disruption
- Short surgical time
- Rapid recovery
- Fewer postoperative complications
Though the pressure reduction may not match trabeculectomy, combining MIGS with cataract surgery provides a dual benefit — restoring vision and controlling IOP simultaneously.
What’s Next in Glaucoma Surgery
The future lies in next-generation stents, sustained-release drug implants, and robotic assistance to achieve precision placement. The focus is shifting from pressure control to neuroprotection and optic nerve preservation.
Conclusion
MIGS represents a paradigm shift — safer, simpler, and more physiologic. It empowers surgeons with more tools and patients with faster, safer options for long-term glaucoma control.