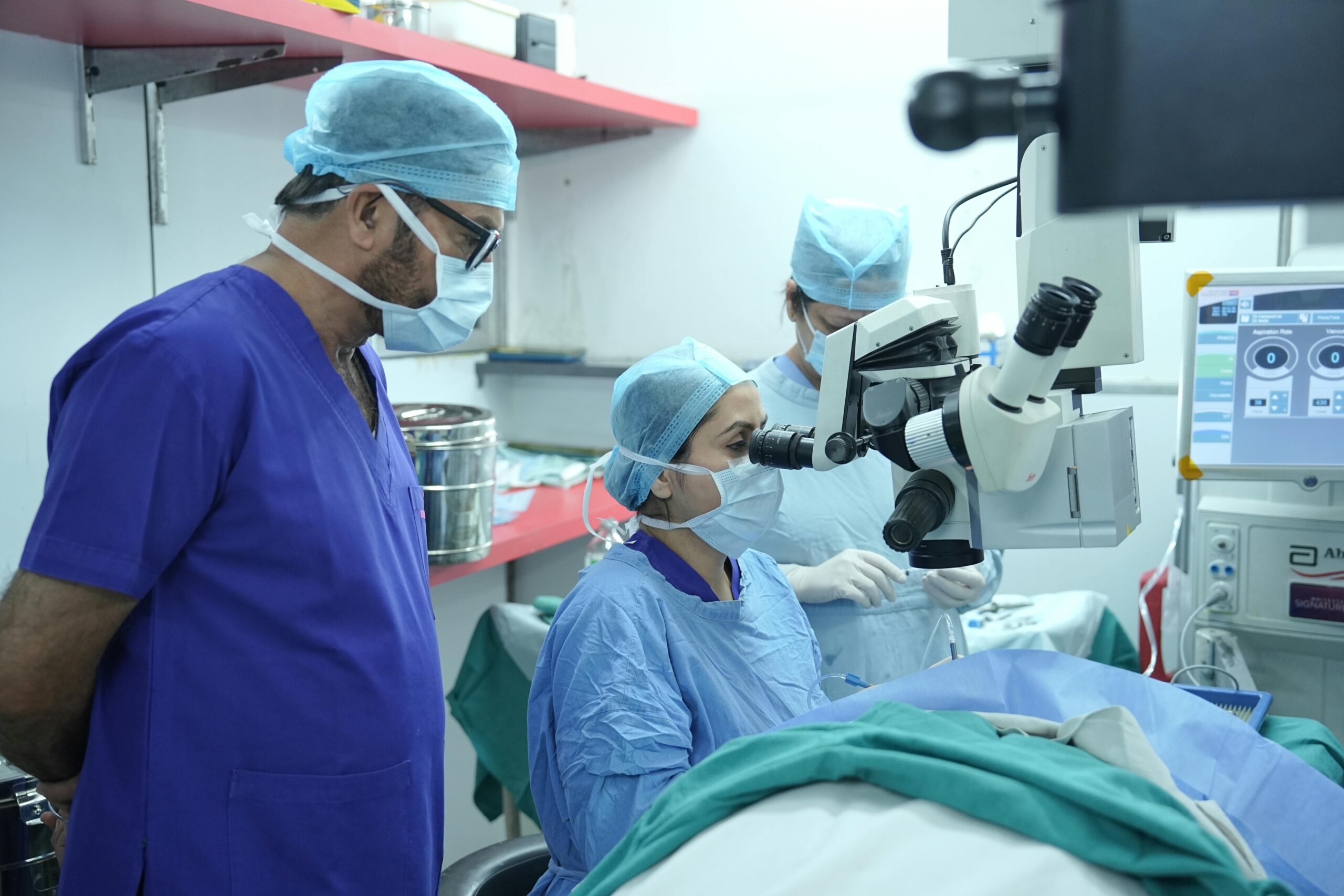
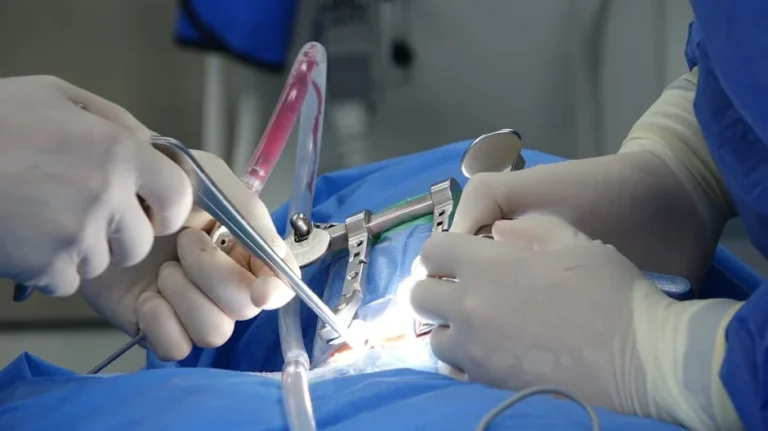
The ocular surface — comprising the cornea, conjunctiva, tear film, and eyelids — plays a vital role in vision and comfort. When disrupted by disease, trauma, or surgery, ocular surface reconstruction can restore both function and clarity.
Common Indications
Ocular surface surgery addresses a variety of conditions:
- Pterygium and conjunctival scarring
- Chemical burns and cicatricial disorders
- Severe dry eye disease
- Corneal ulcers and perforations
- Limbal stem cell deficiency
Pterygium Surgery and Grafting
Modern pterygium surgery favors conjunctival autografts or amniotic membrane grafts, secured with fibrin glue instead of sutures. This reduces recurrence, inflammation, and patient discomfort.
Amniotic Membrane Transplantation
The amniotic membrane has anti-inflammatory, anti-scarring, and epithelial-promoting properties. It’s used for ocular surface healing in burns, ulcers, and persistent epithelial defects. Techniques vary from inlay grafts to overlays depending on the pathology.
Limbal Stem Cell Transplantation
In severe cases of limbal stem cell deficiency, transplantation restores epithelial regeneration. Sources include autologous, allogenic, or cultivated stem cells, representing a key breakthrough in regenerative ophthalmology.
Adjunctive Technologies
Fibrin glue, bioengineered scaffolds, and sutureless techniques have made ocular surface surgery faster and more comfortable. Advances in imaging like anterior segment OCT allow better assessment of the surface and healing progress.
Postoperative Care
Topical antibiotics, steroids, and lubricants are essential for healing. Long-term maintenance of a stable tear film remains crucial for success.
Conclusion
Ocular surface surgery is more than cosmetic repair — it restores the delicate interface that ensures vision clarity and comfort. As bioengineering and cell therapy progress, surgeons are gaining powerful tools to rebuild and rejuvenate the eye’s front line.